7 Common and Serious Side Effects of Airsupra
Understanding Airsupra Side EffectsAirsupra is a prescription inhaler used as a rescue medication to relieve asthma symptoms in adults aged 18 years and older. It is not [...]
Read More
Medically reviewed by Oghenefejiro Okifo | MD, Harvard Medical School | Henry Ford Hospital - Detroit, MI on February 22nd, 2026.
Approximately 10% to 40% of Americans experience sciatica at some point, with lumbar disc herniation responsible for up to 85% of cases
Prolonged sitting, poor lifting form, and sudden physical stress are the most common triggers for flare-ups
Underlying conditions like herniated discs, spinal stenosis, and piriformis syndrome create ongoing vulnerability
Lifestyle factors, including diet, footwear, and sleep quality, directly influence pain intensity
Core strengthening, ergonomic adjustments, and knowing when to seek professional help can prevent future episodes
That shooting pain down your leg isn't random. Sciatica flare-ups follow patterns, and understanding those patterns is the first step toward taking control. Between 10% and 40% of Americans experience sciatica at some point in their lives, making it one of the most common pain conditions. The good news: most triggers are identifiable and often preventable once you know what to look for.
The sciatic nerve is the longest and thickest nerve in the human body. It runs from the lower back through the buttocks and down each leg to the feet. When something compresses or irritates this nerve, pain radiates along its entire path. This explains why lower back problems cause leg pain, numbness, or tingling.
Chronic sciatica is ongoing discomfort that persists for months. Acute flares are sudden, intense episodes that interrupt daily life. Anyone who has experienced episodes of sciatica dreads its potential recurrence. Understanding what causes sciatica to flare up helps people avoid specific triggers and manage their condition more effectively.
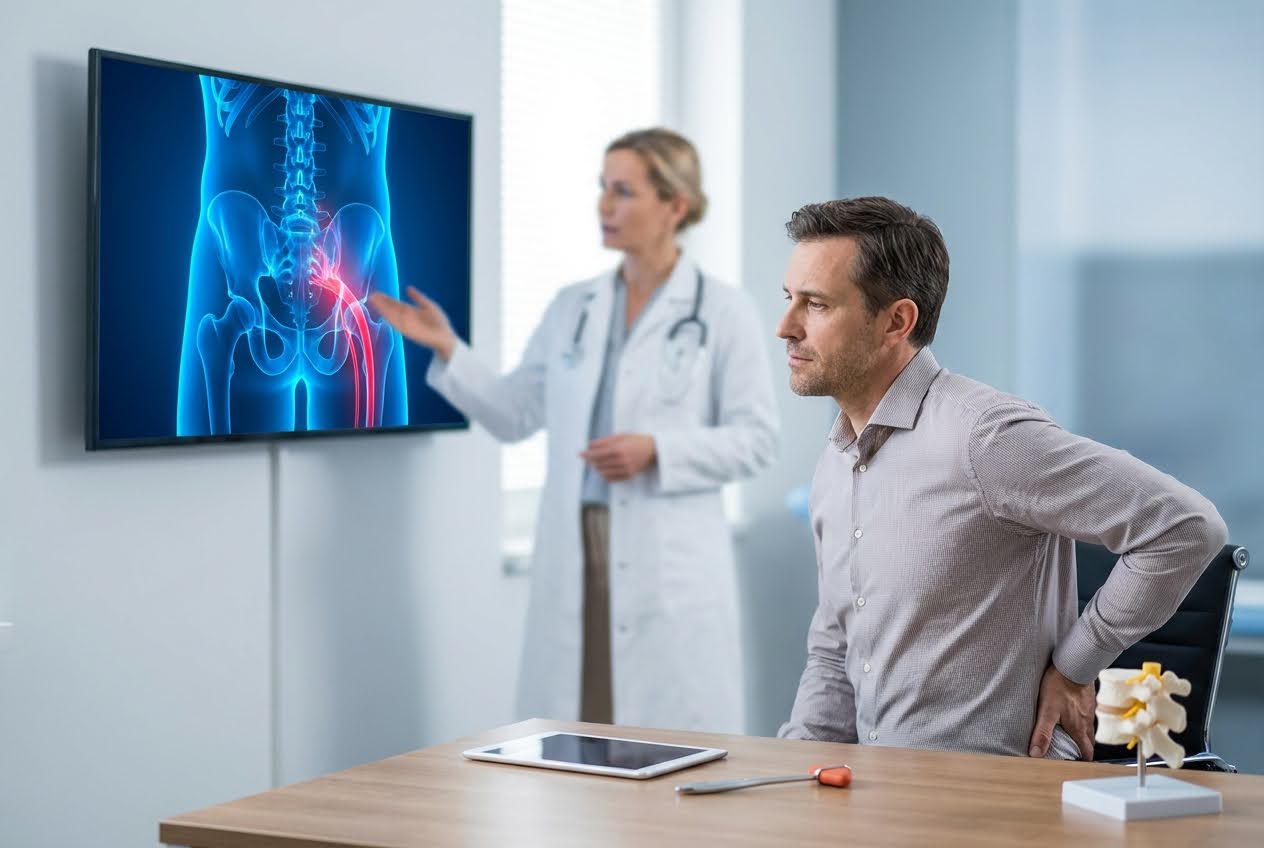 Common Physical Triggers and Mechanical Stress
Common Physical Triggers and Mechanical StressPhysical actions can directly compress the sciatic nerve. These mechanical triggers are the most immediate causes of flare-ups and often the easiest to modify.
Bending at the waist to lift heavy objects compresses spinal discs and strains lower back muscles. This compression can push disc material against the sciatic nerve. Always lift by bending the knees and keeping the back straight. Hold objects close to the body rather than reaching forward.
The increase in sciatica cases correlates with the rise in desk jobs. Sitting for hours puts constant pressure on the lower spine. Slouching makes it worse by flattening the natural lumbar curve. Standing up and moving every 30 minutes significantly reduces this pressure.
Weekend warriors often trigger flare-ups by jumping into intense activity without proper preparation. A sudden twist, an unexpected fall, or pushing too hard during exercise can instantly irritate the sciatic nerve. Gradual warm-ups and awareness of physical limits help prevent many of these episodes.
Some people have structural issues that make their sciatic nerve more vulnerable. These conditions create a baseline of irritation that smaller triggers can easily worsen.
Studies suggest that lumbar disc herniation accounts for approximately 70% to 85% of cases of sciatica. When the soft inner material of a spinal disc pushes through its outer layer, it can press directly on nerve roots. Even small movements can shift this disc material and trigger intense pain.
This condition involves narrowing of the spinal canal in the lower back. The reduced space squeezes nerves, including the sciatic nerve. Walking or standing often worsens symptoms, while sitting or bending forward provides temporary relief.
As people age, spinal discs lose water content and height. This degeneration reduces the intervertebral disc space and can lead to bone spurs that irritate nerves. The condition develops gradually but creates lasting vulnerability to flare-ups.
The piriformis muscle sits deep in the buttocks, and the sciatic nerve runs beneath it. When this muscle tightens or spasms, it can compress the nerve directly. Sitting on hard surfaces or carrying a wallet in a back pocket often aggravates this condition.
Daily habits shape nerve health more than most people realize. Small changes in these areas often produce significant improvements.
Systemic inflammation can exacerbate nerve irritation. Processed foods, excess sugar, and alcohol increase inflammatory responses. Anti-inflammatory foods like fatty fish, leafy greens, and berries help reduce overall inflammation and may decrease flare-up frequency.
High heels shift body weight forward and alter spinal alignment. Worn-out shoes fail to absorb impact during walking. Both situations increase stress on the lower back. Supportive shoes with good arch support protect the spine during daily activities.
Weak core and back muscles cannot properly support the spine. This lack of support allows greater movement between vertebrae, increasing the chance of nerve compression. Regular activity maintains muscle strength and spinal stability.
The mind-body connection plays a real role in sciatica flare-ups. Stress and sleep affect pain perception and muscle tension in measurable ways.
Stress causes muscles to tighten, especially in the back and buttocks. This tension can compress the sciatic nerve or worsen existing irritation. Stress management techniques like deep breathing, meditation, or gentle yoga help relax these muscles.
Poor sleep lowers the body's pain threshold. People who sleep fewer than six hours nightly report more intense pain from the same underlying conditions. Quality sleep facilitates tissue repair and reduces overall pain sensitivity.
Prevention requires consistent effort, but the payoff is significant. These strategies address the root causes of most flare-ups.
Strong abdominal and back muscles act as a natural brace for the spine. Exercises like planks, bridges, and bird-dogs build this protective strength. Stretching the hamstrings, hip flexors, and piriformis muscle maintains flexibility and reduces nerve compression.
Workstation setup matters. Computer screens should be at eye level. Chairs should support the natural curve of the lower back. Standing desks or sit-stand options reduce prolonged sitting. These adjustments remove daily stressors that accumulate over time.
Seek immediate care for severe weakness, loss of bladder or bowel control, or pain that doesn't improve with rest. Doctronic offers free AI doctor visits to assess symptoms and determine whether in-person care is needed. For ongoing management, their telehealth video visits with licensed doctors are available 24/7 in all 50 states.
Most acute flare-ups improve within two to six weeks with appropriate care and activity modification. Mild episodes may resolve in days, while severe ones can persist longer. If pain continues beyond six weeks, professional evaluation is recommended.
Some people report increased pain during cold or damp weather. Cold temperatures may cause muscles to tighten, and barometric pressure changes might affect joint fluid. Staying warm and maintaining activity during weather changes can help.
Prolonged bed rest actually worsens sciatica in most cases. Short rest periods of a few hours are acceptable, but gentle movement promotes healing. Walking and light stretching maintain blood flow and prevent muscle stiffness.
Excess body weight increases spinal pressure and can exacerbate disc problems. Even modest weight loss reduces this load and decreases flare-up frequency. Combined with core strengthening, weight management provides significant protection.
Understanding what causes sciatica to flare up puts control back in your hands. From lifting techniques to sleep habits, most triggers are manageable once identified. For quick guidance on symptoms or treatment options, Doctronic provides instant AI-powered medical insights and affordable telehealth visits with real doctors whenever needed.
Understanding Airsupra Side EffectsAirsupra is a prescription inhaler used as a rescue medication to relieve asthma symptoms in adults aged 18 years and older. It is not [...]
Read MoreUnderstanding Budesonide Interactions for Safe UsageBudesonide is a corticosteroid medication used to treat conditions like asthma, Crohn's disease, and ulcerative [...]
Read MoreUnderstanding Xolair Interactions for Safe UsageXolair (omalizumab) treats severe allergic asthma, chronic hives, and nasal polyps. When starting this medication, patients [...]
Read More