7 Common and Serious Side Effects of Airsupra
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreRoughly 40% of chronic pain patients screen positive for sleep apnea, yet most remain undiagnosed
Oxygen deprivation during sleep can contribute to reduced spinal tissue oxygenation and inflammation
Sleeping on your back worsens both airway collapse and spinal pressure
Poor sleep lowers your pain tolerance, making existing back problems feel worse
Treating sleep apnea with CPAP therapy often reduces chronic pain symptoms
Weight loss and proper sleep positioning can address both conditions at once
Most people treat sleep apnea and chronic back pain as separate issues. They see a sleep specialist for one and a spine doctor for the other. This approach misses something important: these two conditions feed on each other, making both harder to treat in isolation.
The surprising link between sleep apnea and chronic back pain shows up in clinical data. About 30–40% of patients with chronic pain may screen positive for sleep apnea, yet less than a third get formally tested. That means millions of people suffer from back pain without knowing that their breathing problems at night are making it worse. Understanding how these conditions connect opens the door to better treatment for both. Doctronic helps patients identify these hidden connections through comprehensive AI-powered health assessments.
Your spine needs oxygen to stay healthy. When sleep apnea repeatedly cuts off your air supply throughout the night, your entire body suffers - including your back.
The discs between your vertebrae act like cushions. They absorb shock and allow your spine to bend and twist. These discs get their nutrients through a process that depends on good blood flow and oxygen levels. When sleep apnea causes repeated drops in blood oxygen, the discs receive less of what they need to repair themselves.
Over time, oxygen-starved discs break down faster. They lose height, become less flexible, and develop small tears. This damage leads to the kind of chronic back pain that never quite goes away, no matter how many stretches you do.
Sleep apnea triggers inflammation throughout the body. Each time breathing stops and restarts, stress hormones flood the system. These hormones cause swelling throughout the body, including around the spine.
Chronic inflammation makes nerves more sensitive. It also speeds up the breakdown of cartilage and other soft tissues. People with untreated sleep apnea often have higher levels of inflammatory markers in their blood - the same markers found in patients with severe back pain.
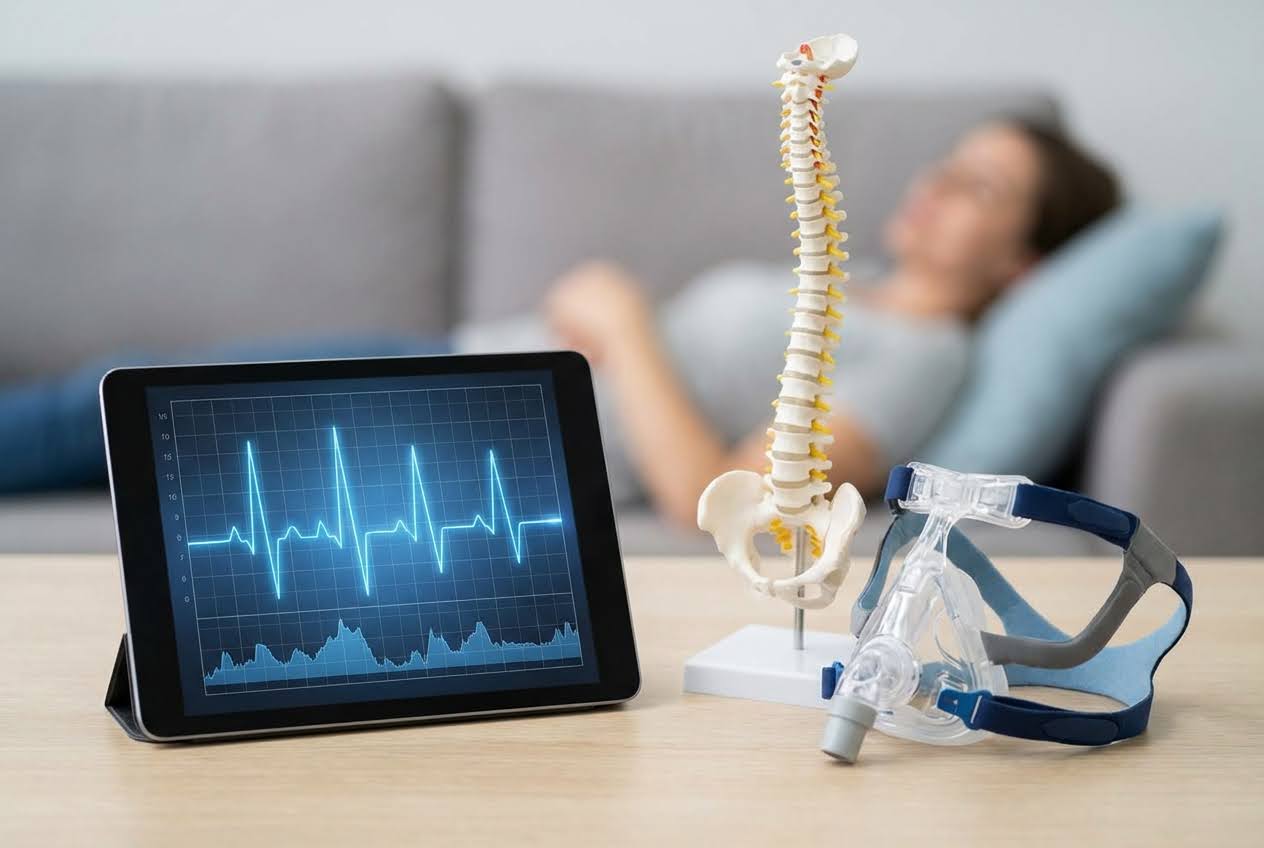 The Bio-Mechanical Impact of Sleep Positions
The Bio-Mechanical Impact of Sleep PositionsHow you sleep matters for both your airway and your spine. The position that feels most natural might actually cause the most problems.
Sleeping flat on your back allows gravity to pull your tongue and soft tissues backward. This narrows the airway, making apnea episodes more frequent and severe. At the same time, sleeping on your back without proper support flattens the natural curve of your lower spine.
This double problem explains why some people wake up with both a sore throat and an aching back. The supine position works against both healthy breathing and healthy spinal alignment.
When breathing becomes difficult during sleep, the body compensates. Neck muscles strain to keep the airway open. Chest muscles work harder to pull air in. This extra effort creates tension that travels down into the upper and middle back.
By morning, muscles that should have relaxed during sleep are tight and sore instead. This tension can exacerbate any existing back problems and trigger new pain patterns.
Sleep apnea doesn't just reduce oxygen - it destroys sleep quality. The constant interruptions prevent the deep, restorative sleep your body needs to manage pain.
When sleep gets disrupted night after night, the nervous system changes. The brain becomes more reactive to pain signals. Small discomforts that would normally go unnoticed start to register as significant pain.
This process is called central sensitization. It explains why people with sleep disorders often develop widespread pain conditions. The brain essentially turns up the volume on pain signals because it never gets the rest it needs to reset.
Many chronic pain sufferers already know: bad sleep makes everything hurt more. Difficulties falling asleep or frequent nighttime waking are often related to poor pain control.
Medical experts note that while sleep apnea may not directly cause back pain, poor sleep can definitely worsen existing back pain. This creates a vicious cycle: pain disrupts sleep, and disrupted sleep amplifies pain.
Sleep apnea and back pain share common causes. Understanding these overlapping risk factors helps explain why the two conditions so often appear together.
Excess weight around the midsection puts pressure on the diaphragm. This large muscle controls breathing. When belly fat restricts diaphragm movement, breathing becomes shallower, and the airway collapses more easily during sleep.
That same abdominal weight also strains the lower back. The spine must work harder to support the extra load, leading to muscle fatigue and disc compression. As of 2026, an estimated 25 million U.S. adults have sleep apnea, but only about 6 million have been formally diagnosed - and obesity remains a major factor in many of these cases.
As people age, tissues throughout the body lose elasticity. In the throat, this means the soft palate and surrounding muscles sag more easily, blocking airflow. In the spine, aging causes discs to dry out and vertebrae to develop bone spurs.
These parallel aging processes explain why both sleep apnea and back pain become more common after age 40. The body's support structures weaken in ways that simultaneously affect breathing and spinal health.
Treating these conditions together produces better results than addressing each one separately. Doctronic can help patients understand which treatment combinations make the most sense for their specific situations.
CPAP machines keep the airway open during sleep by providing continuous air pressure. When patients use CPAP consistently, they experience fewer oxygen drops and better sleep quality. Many report that their chronic pain improves as a result.
The pain reduction happens for several reasons. Better oxygen flow helps tissues heal. Deeper sleep allows the nervous system to reset. Reduced inflammation calms irritated nerves.
Side sleeping with proper pillow support helps both conditions. A pillow between the knees keeps the spine aligned, while side positioning keeps the airway more open than back sleeping.
Adjustable beds that elevate the head slightly can reduce both apnea severity and lower back pressure. Some people benefit from positional therapy devices that prevent them from rolling onto their backs during sleep.
Losing even 10% of body weight can significantly improve sleep apnea. That same weight loss takes pressure off the spine and reduces back pain. Physical therapy strengthens the core muscles that support both good posture and proper breathing mechanics.
A combined approach that addresses weight, posture, and sleep habits produces the best outcomes for people dealing with both conditions.
Sleep apnea doesn't directly cause back pain, but it creates conditions that make back pain worse. Oxygen deprivation, inflammation, and poor sleep quality all increase pain sensitivity and slow tissue healing.
Yes. Given that roughly 30–40% of chronic pain patients screen positive for sleep apnea, testing makes sense for anyone with persistent back problems - especially if you snore, feel tired during the day, or wake up with headaches.
Many patients report reduced back pain after starting CPAP therapy. Better sleep quality and reduced inflammation both contribute to pain relief.
Side sleeping with a pillow between the knees typically works best. This position keeps the airway open while maintaining proper spinal alignment.
Weight loss, physical therapy, proper sleep positioning, and CPAP therapy (if prescribed) can all help both conditions simultaneously. Doctronic offers free AI doctor visits to help you understand your symptoms and develop a treatment plan.
Sleep apnea and chronic back pain often reinforce each other through oxygen deprivation, inflammation, poor sleep quality, and shared risk factors like obesity and aging. Addressing breathing disruptions, sleep position, and weight management can improve both conditions simultaneously. If you struggle with persistent back pain and poor sleep, Doctronic can help you assess symptoms and explore next steps.
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreMeta Description: Learn about 8 budesonide interactions and what to avoid when you’re taking budesonide, including grapefruit and common drugs, to ensure your treatment is [...]
Read MoreMeta Description: Learn about these 7 Xolair interactions and what to avoid when you’re taking Xolair to safely manage your asthma, chronic hives, or nasal polyp [...]
Read More