7 Common and Serious Side Effects of Airsupra
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreApproximately 65% of women aged 60 and older experience high blood pressure, with menopause being a significant trigger due to declining estrogen levels
Estrogen loss causes blood vessels to lose elasticity and become less responsive, indirectly contributing to gradual blood pressure increases
Hot flashes and hypertension symptoms can overlap, making accurate monitoring essential for proper diagnosis
The DASH diet combined with 150 minutes of weekly moderate exercise can reduce blood pressure by approximately 11/5 mmHg
Hormone replacement therapy may help some women, but oral estrogen pills carry higher blood pressure risks than topical forms
doctronic.tech offers convenient telehealth consultations to help women monitor and manage blood pressure changes during menopause
A woman's blood pressure can climb rapidly and unexpectedly during menopause, often catching her completely off guard. One week, the numbers look fine, and the next, they spike into concerning territory. This pattern of sudden high blood pressure during menopause affects millions of women, yet many dismiss the symptoms as typical menopausal discomfort. The reality is that declining hormones fundamentally alter how the cardiovascular system functions. Approximately 65% of women aged 60 and older have high blood pressure. Understanding the connection between hormonal shifts and cardiovascular health can mean the difference between early intervention and serious complications. Women who recognize these changes early and seek guidance through doctronic.tech gain a significant advantage in protecting their long-term health.
Estrogen does far more than regulate reproductive function. This hormone acts as a powerful protector of blood vessel health, keeping arteries flexible and responsive to changes in blood flow. When estrogen levels drop during menopause, blood vessels lose their ability to expand and contract efficiently. Declining estrogen levels cause blood vessels to stiffen and reduce nitric oxide availability, contributing to higher blood pressure over time. The arterial walls become less elastic, forcing the heart to pump harder to move blood through the body.
The sympathetic nervous system controls the body's fight-or-flight response, including heart rate and blood vessel constriction. Estrogen normally helps keep this system balanced. Without adequate estrogen, the sympathetic nervous system becomes overactive, leading to more frequent and intense blood vessel constriction. This explains why many women experience sudden blood pressure spikes during stressful moments that previously caused no cardiovascular response.
Progesterone works alongside estrogen to regulate the body's sodium balance. When progesterone levels fall, the kidneys retain more sodium, which pulls extra fluid into the bloodstream. This increased blood volume raises pressure against arterial walls. Women who never had salt sensitivity before menopause often develop it during this transition.
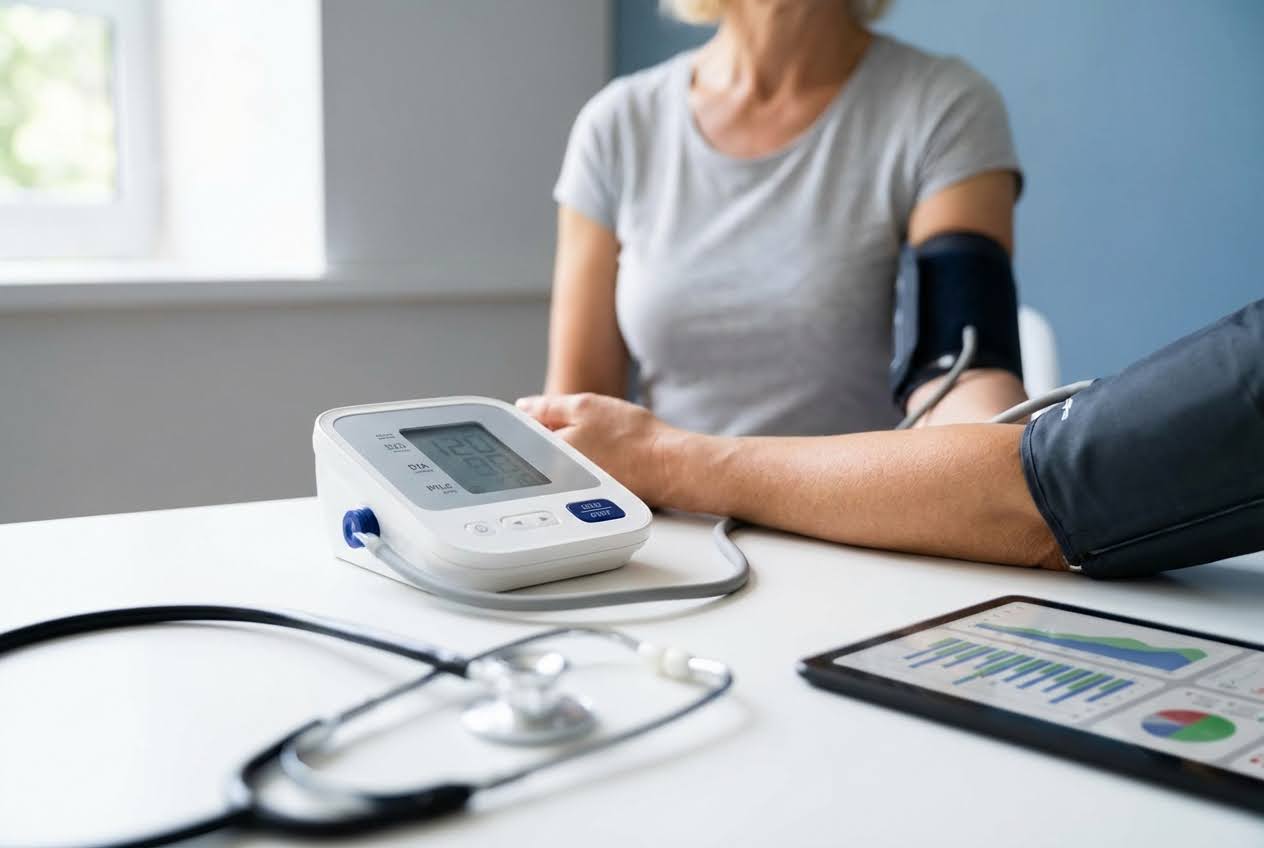 Identifying Symptoms and Warning Signs
Identifying Symptoms and Warning SignsHot flashes and hypertension episodes share overlapping symptoms: facial flushing, sweating, and a racing heart. The key difference lies in timing and triggers. Hot flashes typically last 2 to 4 minutes and occur at random. Blood pressure often spikes during stress, physical exertion, or high-sodium meals. Tracking symptoms with a journal helps identify patterns that distinguish between the two conditions.
Sudden headaches concentrated at the back of the head often signal elevated blood pressure. Dizziness upon standing, visual disturbances, and heart palpitations warrant immediate attention. Many women dismiss these symptoms as normal menopause experiences, delaying critical diagnosis. Any persistent or severe symptoms deserve professional evaluation through a telehealth consultation on doctronic.tech or an in-person visit.
Menopause shifts where the body stores fat, moving it from the hips and thighs to the abdomen. This visceral fat surrounds internal organs and releases inflammatory compounds that damage blood vessels. Even women who maintain a stable weight often experience this redistribution, increasing cardiovascular risk without obvious warning signs.
Sleep apnea rates increase significantly during menopause, as declining hormone levels affect airway muscle tone. Each breathing pause during sleep triggers a stress response that spikes blood pressure. Many women remain undiagnosed because they associate poor sleep with hot flashes rather than breathing problems. Partners who notice snoring or gasping should encourage evaluation.
Menopause often coincides with major life stressors, such as aging parents, career pressures, and changing family dynamics. Chronic stress elevates cortisol, which directly raises blood pressure and promotes abdominal fat storage. The combination of hormonal changes and elevated cortisol creates a particularly damaging environment for cardiovascular health.
Single office readings often miss the full picture. Blood pressure fluctuates throughout the day, and white coat syndrome can produce artificially elevated readings. Ambulatory monitoring tracks pressure over 24 hours, capturing patterns that reveal true cardiovascular status. This method identifies women whose blood pressure spikes only at certain times or during specific activities.
Blood pressure evaluation should include kidney function tests, since the kidneys play a central role in pressure regulation. Lipid profiles reveal cholesterol levels that compound cardiovascular risk. Fasting glucose tests identify insulin resistance, which often accompanies menopausal changes in blood pressure. These tests together provide a complete cardiovascular risk assessment.
The DASH diet emphasizes fruits, vegetables, whole grains, and lean proteins while limiting sodium and processed foods. This eating pattern proves especially effective for menopausal women who develop new sodium sensitivity. Reducing sodium intake to no more than 2,300 mg daily, or ideally around 1,500 mg for those with hypertension, can produce blood pressure reductions comparable to medication in some women.
Both exercise types lower blood pressure, but combining them produces superior results. 150 minutes per week of moderate-intensity aerobic exercise can reduce blood pressure by approximately 11/5 mmHg. Strength training builds muscle mass, improving metabolic function and helping counteract menopausal weight redistribution. Aim for 2 strength sessions and 150 minutes of cardio per week.
HRT can help some women manage blood pressure by restoring estrogen's protective effects on blood vessels. The delivery method matters significantly. Women who take estrogen hormone pills may be more likely to develop high blood pressure compared to those using topical or vaginal forms because oral estrogens are metabolized through the liver. Transdermal patches and gels bypass liver metabolism and carry lower cardiovascular risks.
When lifestyle changes prove insufficient, several medication classes effectively treat menopausal hypertension. ACE inhibitors and ARBs protect kidney function while lowering pressure. Calcium channel blockers help blood vessels relax. Thiazide diuretics reduce fluid volume. The best choice depends on individual health factors, other medications, and specific blood pressure patterns identified through monitoring.
Yes. Women with completely normal blood pressure throughout their lives can develop hypertension during menopause due to hormonal changes affecting blood vessel function and sodium regulation.
Any reading consistently above 120/80 mmHg warrants attention for lifestyle modification, while sustained readings above 130/80 mmHg require medical evaluation. Sudden spikes above 180/120 mmHg require immediate medical evaluation to rule out hypertensive crisis.
Not necessarily. Transdermal estrogen delivery methods carry lower blood pressure risks than oral pills. Individual responses vary, making monitoring essential during HRT.
Take readings at the same times daily, preferably morning and evening, while seated and relaxed. Record numbers in a journal or app for at least two weeks before medical appointments.
Many women achieve significant reductions in blood pressure through weight loss, particularly by losing visceral abdominal fat. A 10-pound loss can reduce systolic pressure by around 5 mmHg.
Sudden high blood pressure during menopause is common and often linked to declining estrogen, increased arterial stiffness, and changes in sodium regulation. Because symptoms can overlap with hot flashes, consistent monitoring is essential. Lifestyle strategies like the DASH diet and regular exercise are highly effective, and medications or tailored HRT may help when needed. doctronic.tech offers convenient telehealth support to guide evaluation and management.
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreMeta Description: Learn about 8 budesonide interactions and what to avoid when you’re taking budesonide, including grapefruit and common drugs, to ensure your treatment is [...]
Read MoreMeta Description: Learn about these 7 Xolair interactions and what to avoid when you’re taking Xolair to safely manage your asthma, chronic hives, or nasal polyp [...]
Read More