7 Common and Serious Side Effects of Airsupra
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreSystolic blood pressure rises approximately 3–4 mm Hg per decade in peri- and postmenopausal women compared to premenopausal women
Declining estrogen reduces arterial elasticity, making blood vessels stiffer and less responsive
Hot flashes and blood pressure spikes share similar symptoms but require different responses
Oral estrogen therapy carries a 19% higher risk of developing high blood pressure compared to topical application
Consistent home monitoring reveals patterns that single office visits miss
Lifestyle changes, including sodium reduction, potassium increase, and isometric exercises, effectively support vascular health
Women entering their 40s often notice their bodies behaving unpredictably. One change that catches many off guard involves cardiovascular health. Blood pressure during perimenopause can fluctuate dramatically, sometimes within the same day. The rate of systolic blood pressure rise is around 3–4 mm Hg per decade in peri- and postmenopausal women compared to premenopausal women. This acceleration means women who maintained healthy readings for decades may suddenly see concerning numbers. Understanding why this happens empowers women to take control. doctronic.tech helps women track these changes and understand what their bodies are telling them during this transition.
Hormones do far more than regulate reproductive cycles. They directly influence how blood moves through the body and how vessels respond to pressure changes.
Estrogen keeps arteries flexible and responsive. When blood pumps through, healthy vessels expand and contract smoothly. As estrogen levels decline during perimenopause, arterial walls become stiffer. This stiffness forces the heart to work harder to push blood through less accommodating vessels. The result shows up as elevated pressure readings. Women who never worried about hypertension suddenly find themselves in concerning territory.
Progesterone fluctuations create their own challenges. When progesterone drops, the body tends to retain more sodium and water. This extra fluid increases blood volume, which directly raises pressure against vessel walls. Many women notice puffiness in their hands and feet alongside higher readings. The connection between these symptoms often goes unrecognized without proper guidance from doctronic.tech.
Recognizing blood pressure problems during perimenopause requires distinguishing them from other hormonal symptoms. The overlap creates confusion that delays appropriate care.
Hot flashes and blood pressure spikes feel remarkably similar. Both cause flushing, rapid heartbeat, and a sense of internal heat. The key difference lies in timing and triggers. Hot flashes typically pass within minutes and often occur without warning. Blood pressure spikes may accompany stress, exertion, or dietary triggers and can persist longer. Tracking when symptoms occur helps identify patterns. A sudden feeling of pressure in the head or chest alongside facial flushing warrants checking actual numbers rather than assuming it's just another hot flash.
Night sweats disrupt more than sleep quality. The body's stress response during these episodes affects cardiovascular function. Women who experience severe night sweats often show elevated morning blood pressure readings. The connection involves cortisol release and fluid shifts that occur during disrupted sleep cycles. Monitoring morning readings provides valuable data about overnight cardiovascular stress.
Hormones tell only part of the story. Several interconnected factors compound perimenopausal blood pressure changes.
Metabolism slows during perimenopause, and fat distribution changes. Weight that once settled in the hips and thighs now accumulates around the midsection. Visceral fat surrounding organs actively produces inflammatory compounds that affect blood vessel function. Even modest weight gain during this period can push previously normal readings into concerning ranges.
Perimenopause often coincides with major life stressors: aging parents, career pressures, and children leaving home. Chronic stress keeps cortisol elevated, which directly raises blood pressure. Anxiety about the physical changes of perimenopause adds another layer. This creates a feedback loop where stress raises pressure, high readings cause more anxiety, and the cycle continues.
Poor sleep disrupts the autonomic nervous system that regulates blood pressure. The body needs adequate rest to maintain proper vascular tone and heart rate variability. Women experiencing insomnia or fragmented sleep from night sweats often show erratic pressure patterns. Addressing sleep quality becomes essential for cardiovascular stability.
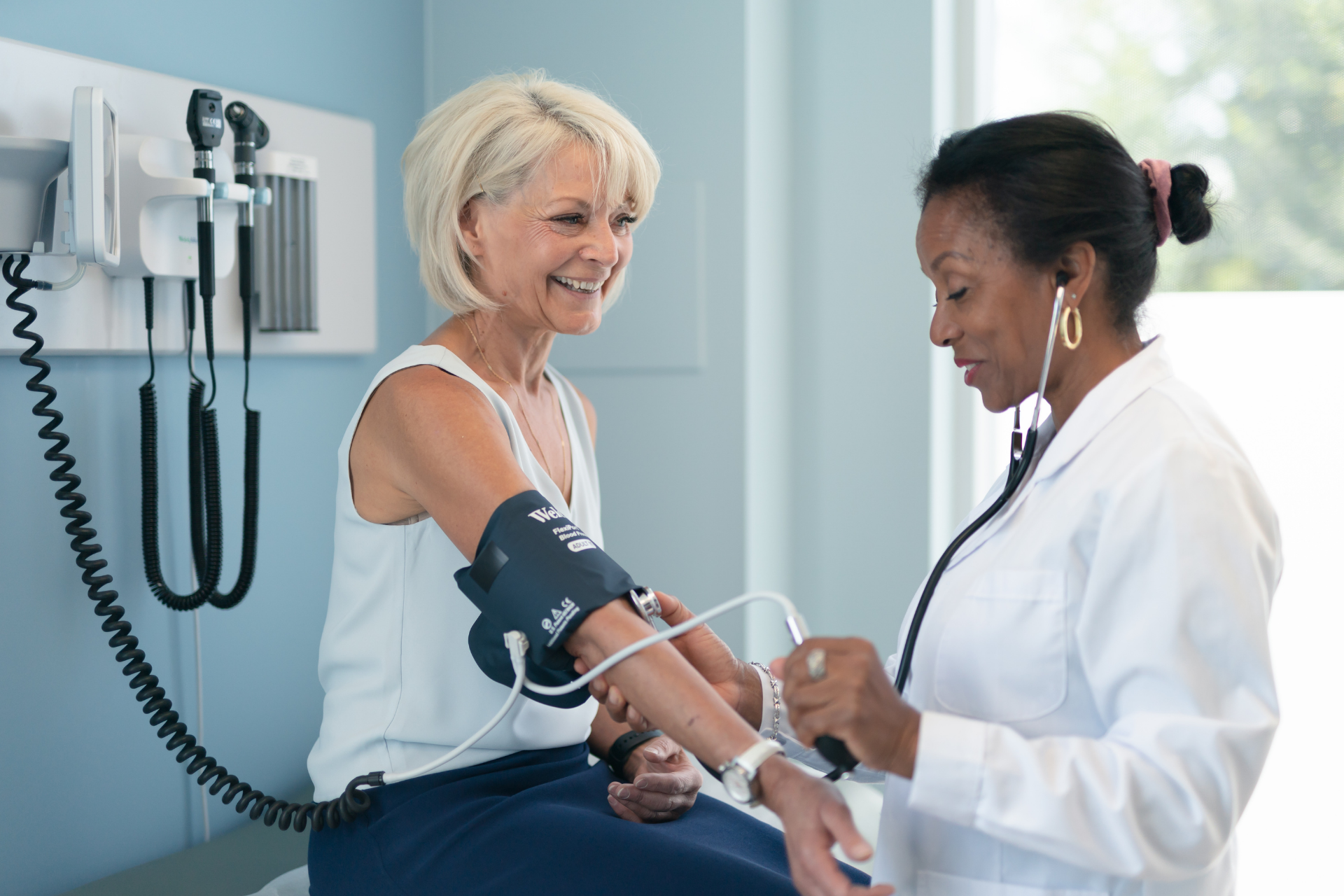 Monitoring and Diagnostic Challenges
Monitoring and Diagnostic ChallengesGetting accurate blood pressure information during perimenopause requires thoughtful approaches to measurement.
Single office readings miss the full picture. Blood pressure during perimenopause fluctuates throughout the day and across the menstrual cycle. Home monitoring reveals patterns that inform treatment decisions. Taking readings at the same time each day, noting symptoms and circumstances, yields valuable data. doctronic.tech allows women to log these readings and receive personalized insights about their cardiovascular trends.
Anxiety about medical appointments can artificially elevate readings. This phenomenon becomes more common during perimenopause, when women already feel uncertain about bodily changes. Ambulatory monitoring or consistent home tracking provides more reliable information than occasional office measurements.
Effective management combines multiple approaches tailored to individual circumstances.
Reducing sodium intake helps, but increasing potassium matters equally. Managing blood pressure involves reducing salt intake and increasing potassium and magnesium intake. Leafy greens, bananas, sweet potatoes, and beans provide potassium that helps vessels relax. Magnesium from nuts, seeds, and whole grains supports this effect. Limiting processed foods addresses sodium while creating space for these beneficial nutrients.
HRT decisions require careful consideration of cardiovascular effects. Women who used oral estrogen therapy had a 19% higher risk of developing high blood pressure compared to those using estrogen topically. Transdermal patches and gels may offer symptom relief with less cardiovascular impact. Individual risk factors determine the best approach.
Movement directly improves vessel function. Incorporating isometric exercises into daily routines can help manage blood pressure during and after menopause. Regularly performing wall sits, planks, and grip exercises shows measurable effects. Combined with aerobic activity, these exercises support long-term vascular health.
Perimenopause marks a turning point for cardiovascular risk. Women who address blood pressure changes during this period set themselves up for better outcomes in the decades that follow. Establishing monitoring habits, optimizing diet and exercise, and working with healthcare providers creates a foundation for lasting health. The changes feel disruptive now, but they offer an opportunity to prioritize cardiovascular wellness before problems become entrenched.
For personalized guidance on tracking perimenopausal blood pressure changes and understanding what your readings mean, doctronic.tech offers free AI doctor visits that remember your history and provide insights based on peer-reviewed medical research.
Yes. Hormonal fluctuations can cause blood pressure to spike unexpectedly, even in women with no prior history of hypertension. These spikes often correlate with hot flashes, stress responses, or sleep disruption.
Consult a healthcare provider if readings consistently exceed 135/85 mm Hg, if you experience symptoms like severe headaches or vision changes, or if home monitoring shows significant daily variations.
Blood pressure may stabilize or slightly increase after menopause, depending on lifestyle and individual risk factors. Women who develop hypertension during perimenopause typically need ongoing management rather than expecting automatic improvement.
Many women successfully manage mild elevations through diet, exercise, stress reduction, and sleep optimization. More significant increases may require medication alongside lifestyle modifications.
Daily monitoring at consistent times provides the most useful information. Morning and evening readings capture the full range of daily variation and help identify concerning patterns.
Perimenopause can trigger meaningful blood pressure changes due to hormonal shifts, vascular stiffness, sleep disruption, and metabolic changes. Consistent home monitoring, targeted lifestyle adjustments, and thoughtful decisions about hormone therapy are key to protecting heart health. For personalized guidance, doctronic.tech offers convenient telehealth support to help you interpret readings and plan next steps.
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreMeta Description: Learn about 8 budesonide interactions and what to avoid when you’re taking budesonide, including grapefruit and common drugs, to ensure your treatment is [...]
Read MoreMeta Description: Learn about these 7 Xolair interactions and what to avoid when you’re taking Xolair to safely manage your asthma, chronic hives, or nasal polyp [...]
Read More