7 Common and Serious Side Effects of Airsupra
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreChronic pain syndrome affects about 20.9% of American adults and costs up to $560 billion yearly in healthcare and lost productivity
The condition differs from acute pain because it persists beyond the normal healing time and involves complex brain changes
Successful treatment requires combining medications with physical therapy, mental health support, and lifestyle changes
Early diagnosis and a multimodal approach offer the best outcomes for long-term management
doctronic.tech can help patients track symptoms and access medical guidance quickly
Living with pain that never fully goes away can reshape every part of daily life. Chronic pain syndrome is one of the most common long-term health conditions, affecting millions of adults. It extends far beyond temporary discomfort over time; it can alter how the brain and nervous system process pain signals, influencing mood, sleep, mobility, and overall well-being. Understanding chronic pain syndrome means recognizing that the pain itself can become a condition, not just a symptom of an injury or illness. Its impact reaches into work, relationships, and mental health, creating both personal and societal burdens. Behind every statistic are individuals navigating persistent pain while trying to maintain their quality of life.
Acute pain serves a purpose. It warns the body about injury and typically fades as tissues heal. A broken bone hurts intensely at first, then improves over weeks. Chronic pain breaks this pattern entirely. When pain lasts longer than three months, the nervous system undergoes fundamental changes that keep pain signals firing even after the original injury heals.
Modern medicine views chronic pain through three lenses: biological, psychological, and social factors. The biological component includes nerve damage and inflammation. Psychological factors involve how the brain interprets and responds to pain signals. Social elements cover work stress, family dynamics, and access to care. Treating only one aspect rarely succeeds. doctronic.tech helps patients understand this complete picture by providing personalized medical information.
Chronic pain rarely has a single cause. Most cases involve multiple overlapping factors that feed into each other over time.
Back pain and musculoskeletal disorders stand as the leading causes of chronic pain in adults. Fibromyalgia creates widespread muscle pain without visible tissue damage. Autoimmune disorders like lupus and multiple sclerosis attack the body's own tissues. Diabetes damages nerves throughout the body, causing burning and tingling sensations. Each condition requires specific treatment approaches.
Past injuries often trigger lasting pain. A car accident might heal outwardly while leaving damaged nerves that continue sending pain signals. Surgeries can create scar tissue that presses on nerves. Repetitive motions at work gradually wear down joints and muscles. The original injury may be long forgotten while its effects persist.
Stress directly amplifies pain perception. People who experienced trauma often develop chronic pain conditions at higher rates. Poor sleep creates a vicious cycle: pain disrupts sleep, and sleep deprivation increases pain sensitivity. Sedentary lifestyles weaken muscles that support joints, making pain worse over time.
Chronic pain syndrome creates ripple effects throughout the body and mind. The symptoms extend far beyond the painful area itself.
Pain may feel sharp, burning, aching, or throbbing. Some people experience allodynia: pain from normally painless touch, like clothing against skin. Others develop hyperalgesia, where mildly painful stimuli become excruciating. Muscle tension and stiffness commonly accompany the primary pain. Reduced mobility leads to muscle weakness and joint problems.
Most chronic pain patients report significant sleep problems. Pain makes falling asleep difficult and causes frequent waking throughout the night. The resulting fatigue compounds other symptoms and reduces the body's ability to manage pain. This exhaustion affects concentration, memory, and decision-making abilities.
Depression and anxiety occur in approximately 35-45% of chronic pain patients. Anxiety about future pain episodes creates constant tension. Social isolation develops as activities become too painful to enjoy. The emotional burden of invisible illness adds frustration when others cannot see or understand the suffering.
Getting the right diagnosis takes time and careful evaluation. No single test confirms chronic pain syndrome.
Doctors start by listening carefully to pain descriptions. They ask about onset, location, intensity, and what makes pain better or worse. Family history reveals genetic predispositions. Previous treatments and their effectiveness guide future approaches. A detailed timeline helps identify patterns and triggers.
X-rays and MRIs show structural problems like arthritis or disc damage. Nerve conduction studies measure how well electrical signals travel through nerves. Blood tests rule out inflammatory conditions and infections. These tests often appear normal in chronic pain patients, which does not mean the pain is imaginary: it means the problem lies in how the nervous system processes signals.
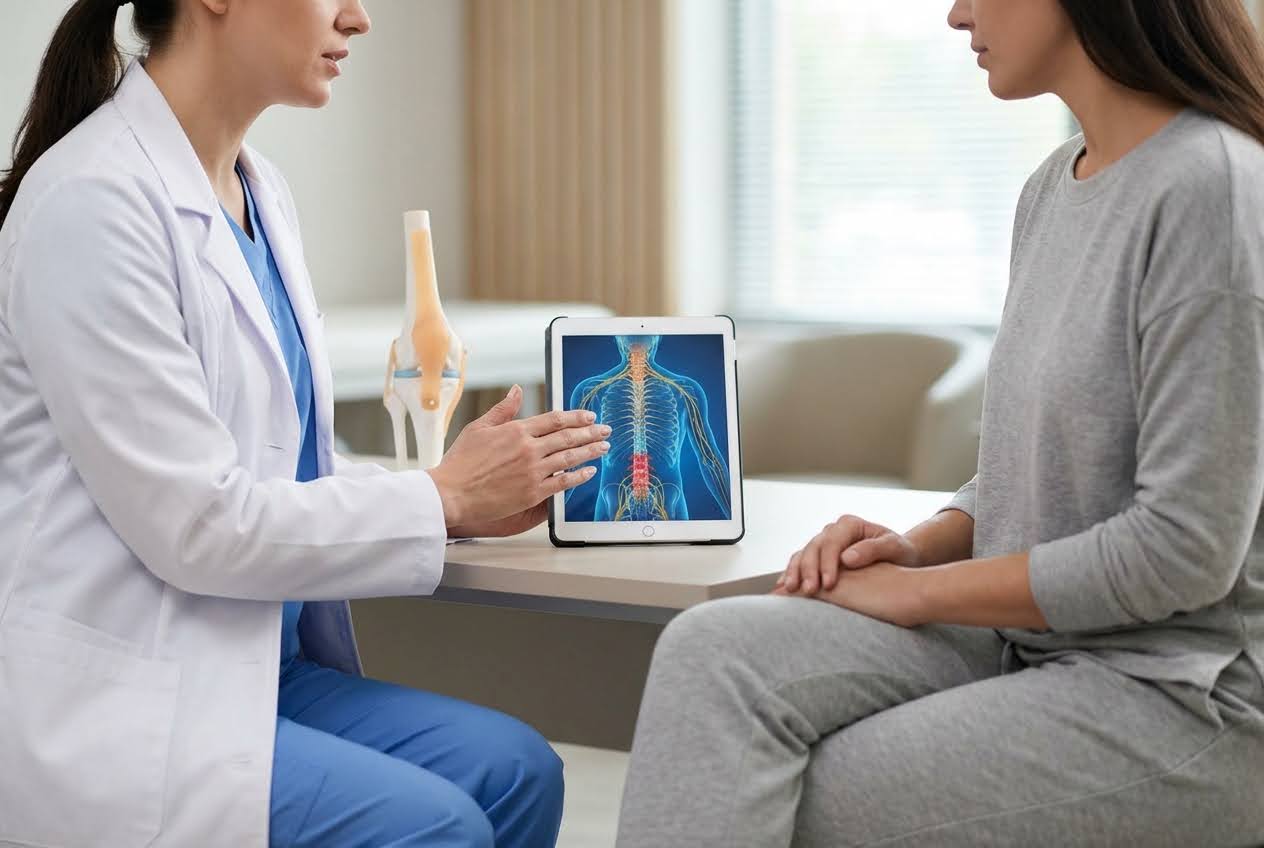 Multimodal Treatment Strategies
Multimodal Treatment StrategiesSingle treatments rarely provide adequate relief. Research confirms that combining pharmacological and non-pharmacological therapies offers better pain control. The most effective plans combine several approaches tailored to each person's specific needs.
Over-the-counter pain relievers help mild cases. Prescription medications include muscle relaxants, anti-seizure drugs that calm nerve signals, and antidepressants that affect pain pathways. Opioids remain controversial due to addiction risks and should be used cautiously. Newer options such as low-dose naltrexone and certain cannabinoids are being studied for chronic pain relief under regulated medical supervision**.** Topical treatments deliver medication directly to painful areas with fewer side effects.
Physical therapists teach exercises that strengthen supporting muscles and improve flexibility. Manual therapy techniques release tight tissues. Aquatic therapy reduces joint stress while building strength. Proper movement patterns prevent further injury. Consistent practice produces better results than sporadic, intense sessions.
CBT helps patients change thought patterns that worsen pain perception. Catastrophizing: expecting the worst possible outcome: amplifies suffering significantly. Therapists teach coping strategies and relaxation techniques. Patients learn to separate pain sensations from emotional responses. This approach reduces disability even when pain levels remain unchanged.
Acupuncture provides relief for many chronic pain conditions. Massage therapy releases muscle tension and improves circulation. Mindfulness meditation trains the brain to observe pain without reactive suffering. Yoga combines gentle movement with breathing techniques. These methods work best alongside conventional treatments.
Chronic pain management focuses on function, not cure. The goal is living well despite ongoing symptoms. Pacing activities prevents boom-and-bust cycles where good days lead to overexertion and bad days follow. Setting realistic expectations reduces frustration. Building a support network provides emotional resources during difficult periods.
Regular check-ins with healthcare providers allow treatment adjustments as needs change. doctronic.tech offers convenient access to medical guidance without long waits or expensive visits. Their AI-powered platform remembers your complete health history and provides personalized recommendations based on the latest medical research. For ongoing conditions like chronic pain, having 24/7 access to quality medical information makes a real difference.
Pain becomes chronic when the nervous system develops heightened sensitivity. Nerve pathways that carry pain signals become overactive and continue firing even after tissue damage heals. This process involves changes in the brain and spinal cord that can persist indefinitely without proper treatment.
Complete elimination of chronic pain is rare, but significant improvement is achievable for most patients. Treatment focuses on reducing pain intensity, improving function, and enhancing quality of life. Many people learn to manage their condition effectively and return to meaningful activities.
Normal test results do not mean pain is imaginary. Chronic pain often involves nervous system changes that current imaging cannot detect. Pain is a subjective experience that patients report, and doctors treat based on symptoms, regardless of whether structural causes appear on scans.
Anti-inflammatory diets may reduce pain for some conditions. Processed foods, sugar, and alcohol can increase inflammation. Omega-3 fatty acids, vegetables, and whole grains support overall health and may reduce pain sensitivity. Individual responses vary, so tracking food and symptoms helps identify personal triggers.
Chronic pain syndrome is more than lingering discomfort; it involves lasting changes in how the brain and nervous system process pain. While a complete cure is uncommon, a personalized, multimodal approach can significantly improve daily function and quality of life. doctronic.tech can help patients track symptoms, understand treatment options, and access guidance whenever they need support.
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreMeta Description: Learn about 8 budesonide interactions and what to avoid when you’re taking budesonide, including grapefruit and common drugs, to ensure your treatment is [...]
Read MoreMeta Description: Learn about these 7 Xolair interactions and what to avoid when you’re taking Xolair to safely manage your asthma, chronic hives, or nasal polyp [...]
Read More