7 Common and Serious Side Effects of Airsupra
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreAnxiety and back pain share a two-way connection through stress hormones, muscle tension, and brain chemistry changes
About 20 million Americans live with both chronic pain and anxiety symptoms at the same time
Stress causes muscles to tighten and stay tight, leading to real physical pain in the back
Fear of pain can make people avoid movement, which actually makes back problems worse
Treatments that address both mind and body work better than treating just one condition
doctronic.tech offers 24/7 access to doctors who can help with both anxiety and back pain concerns
Your back hurts. You also feel constantly on edge. These two problems may seem unrelated, but they are closely connected. Millions of people live with chronic pain alongside anxiety and depression symptoms. The relationship works both ways: stress and anxiety can intensify back pain, and ongoing back pain can fuel worry and emotional distress. Low back pain is one of the most common health conditions worldwide, and its impact continues to grow. Understanding how your mind influences your spine is the first step toward meaningful relief. The encouraging news is that treating anxiety and back pain together is far more effective than addressing either one alone.
The connection between your brain and your back is real and measurable. Scientists have found clear pathways that explain why worry shows up as physical pain.
When you feel anxious, your body releases a stress hormone called cortisol. Short bursts of cortisol help you handle danger. But when anxiety sticks around for weeks or months, cortisol stays high. This can contribute to inflammation throughout your body, including in your spine. Inflamed tissues may swell and press on nerves. The result is pain that feels very real because it is real. Your back is not making things up. While cortisol itself does not directly cause physical damage to tissues, chronic stress and elevated cortisol can, over time, indirectly worsen inflammation and pain sensitivity.
Anxious people hold their muscles tight without knowing it. This is called muscle guarding. Your body thinks danger is near, so it prepares to fight or run. The muscles in your back, neck, and shoulders stay clenched for hours. After days or weeks, these muscles become sore and stiff. Many people discover they have been holding tension only after a massage therapist points it out. doctronic.tech can help identify whether your back pain might be connected to stress patterns through a free AI consultation.
Anxiety changes how your brain processes pain signals. A process called central sensitization makes your nervous system extra sensitive. Normal sensations that should not hurt start to feel painful. Your brain turns up the volume on pain signals. This means the same back problem feels much worse when you are anxious than when you are calm. The pain is not imaginary, but anxiety is making it stronger than it needs to be.
Not all back pain comes from stress, but certain patterns suggest anxiety plays a role. Knowing these signs helps you find the right treatment.
Stress-related pain often settles between the shoulder blades and at the base of the neck. People describe it as a tight band or heavyweight. The pain gets worse during stressful times at work or home. It may ease on weekends or vacations. If your upper back pain follows your stress levels, anxiety is likely involved. Heat, stretching, and relaxation often help more than pain pills for this type of discomfort.
Some people experience sudden lower back spasms during or after panic attacks. The intense muscle tightening of a panic episode can trigger painful cramps in the lower spine. These spasms may last minutes or hours. They often happen without any injury or physical strain. If your back "goes out" during times of high anxiety, the connection is probably not a coincidence.
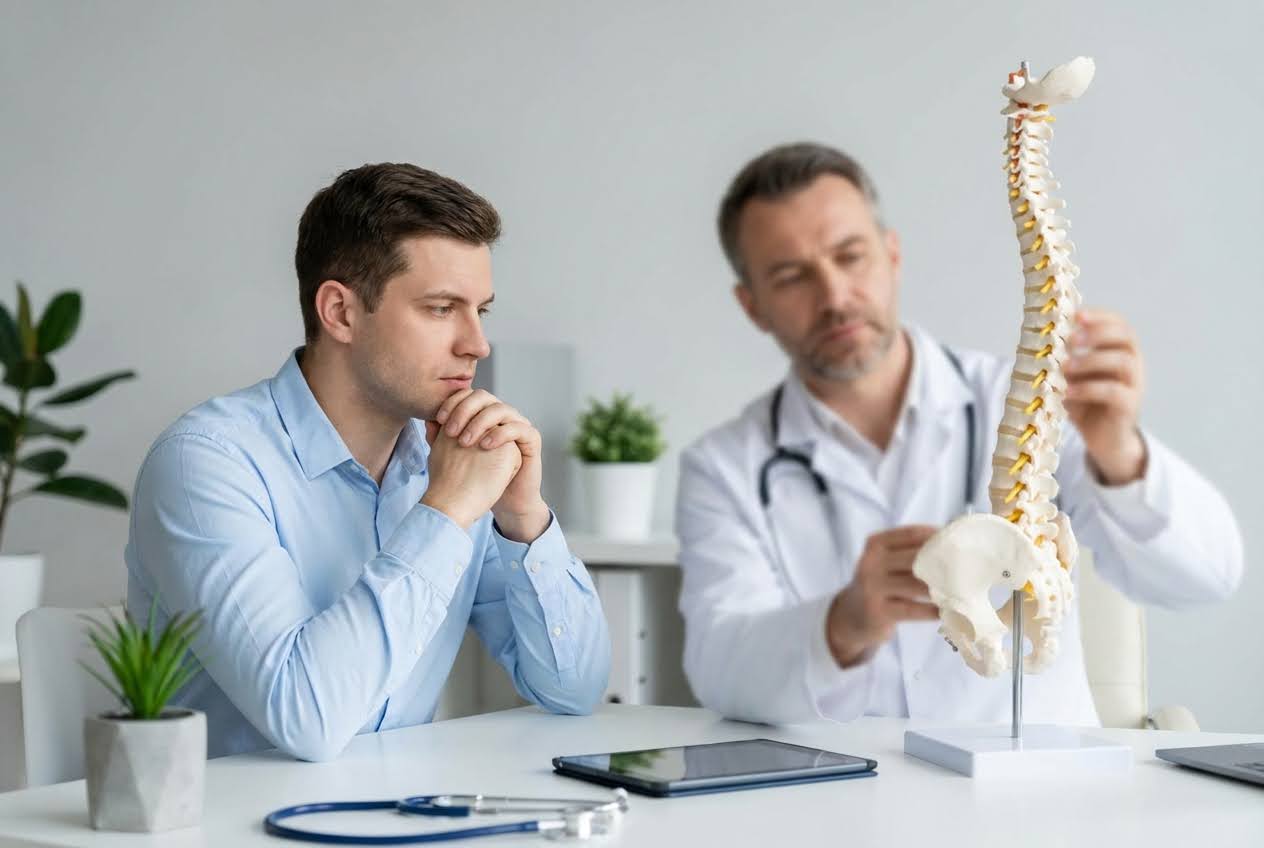 The Psychological Feedback Loop of Chronic Pain
The Psychological Feedback Loop of Chronic PainPain and anxiety feed each other in a vicious cycle. Breaking this loop requires understanding how it works.
When your back hurts, you naturally want to avoid movements that cause pain. This makes sense at first. But avoiding all movement leads to weak muscles. Weak muscles cannot support your spine properly. This causes more pain, which leads to more avoidance. Soon, you are trapped in a cycle of fear and weakness. Use fear; don't let it use you. Take some breaths and relax. Be mindful of any tension, uneasiness, or worry. The path out of this cycle requires gentle, gradual movement despite the fear.
Catastrophizing means assuming the worst about your pain. A twinge becomes proof of a serious injury. Mild discomfort becomes unbearable suffering in your mind. This thinking pattern is common in anxious people. The problem is that expecting terrible pain actually makes pain feel worse. Your brain prepares for disaster and interprets normal signals as dangerous. Learning to notice these thought patterns is the first step toward changing them.
Treating anxiety and back pain together produces better results than treating either alone. Several approaches work well.
CBT teaches you to notice and change unhelpful thought patterns. A therapist helps you identify catastrophic thinking and replace it with balanced thoughts. CBT also includes gradual exposure to feared movements. Studies show CBT reduces both pain intensity and anxiety levels. Many people see improvement within 8 to 12 sessions. This approach treats the root cause rather than just covering up symptoms.
Mindfulness teaches you to observe pain without fighting it. This sounds strange, but fighting pain often makes it worse. Accepting sensations as they are reduces suffering. Yoga combines mindfulness with gentle movement. The stretching releases tight muscles while the breathing calms the nervous system. Regular practice rewires how your brain responds to stress. doctronic.tech can provide personalized recommendations for mindfulness and movement programs based on your specific symptoms.
Slow, deep breathing tells your body the danger has passed. This switches off the stress response and allows muscles to relax. Try breathing in for four counts, holding for four counts, and breathing out for six counts. Do this for five minutes when you notice tension building. The effects are immediate and measurable. Your heart rate slows, your muscles soften, and pain often decreases within minutes.
Some situations require professional help. Seek care if your pain lasts more than a few weeks, wakes you from sleep, or comes with numbness or weakness. Mental health support is important if anxiety interferes with daily life or if you feel hopeless. A doctor can rule out serious spine problems and suggest appropriate treatment. A therapist can address the anxiety component. Many people benefit from seeing both types of providers.
Yes. Chronic muscle tension, inflammation from stress hormones, and central sensitization can all create real back pain without any injury to the spine.
Stress-related pain often moves around, gets worse during anxious times, and improves with relaxation. Physical injuries usually hurt in one specific spot and do not change with mood. A doctor can help determine the cause.
For many people, yes. Reducing anxiety often reduces pain significantly. Some people find that their back pain disappears entirely once their anxiety is under control.
Deep breathing exercises and gentle stretching often provide quick relief. Heat applied to tense muscles also helps. These methods work within minutes for many people.
Gentle movement usually helps more than rest. Walking, swimming, and yoga are good choices. Avoiding all activity often makes both anxiety and back pain worse over time.
Anxiety and back pain are deeply connected through stress hormones, muscle tension, and brain chemistry. Treating both conditions together works better than addressing either one alone. For quick answers about your symptoms, visit doctronic.tech for a free AI consultation or affordable video visits with real doctors, available 24/7 in participating U.S. states.
Meta Description: Learn about the 7 common and serious side effects of Airsupra and how to manage risks like oral thrush or heart issues through proper inhaler [...]
Read MoreMeta Description: Learn about 8 budesonide interactions and what to avoid when you’re taking budesonide, including grapefruit and common drugs, to ensure your treatment is [...]
Read MoreMeta Description: Learn about these 7 Xolair interactions and what to avoid when you’re taking Xolair to safely manage your asthma, chronic hives, or nasal polyp [...]
Read More